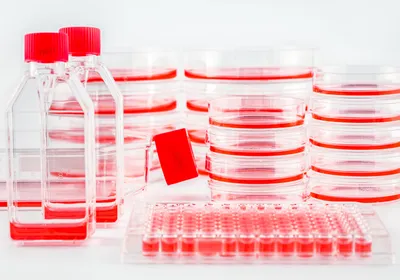
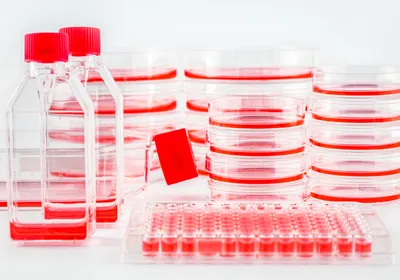
ABOVE: Illustration of a mitochondrion. A genetic variant in the mitochondrial genome is responsible for Leber hereditary optic neuropathy.
© ISTOCK.COM, TUSSIK1
I
n a Phase 3 gene therapy trial intended to improve vision among patients with Leber hereditary optic neuropathy, recipients gained somewhat better sight in both eyes even though only one was treated. The results and an investigation into possible explanations for the findings were published December 9 in Science Translational Medicine.
The paper “has very strong clinical implications that a single injection maybe is enough for bilateral effects,” says Thomas Corydon, who studies ocular gene therapy at Aarhaus University in Denmark and was not involved in the work.
The onset of Leber hereditary optic neuropathy (LHON) is sudden. Patients—usually young men—start losing vision at the center of one eye. Within months, the other eye follows, leaving them legally blind. The disease is caused by a point mutation in ...