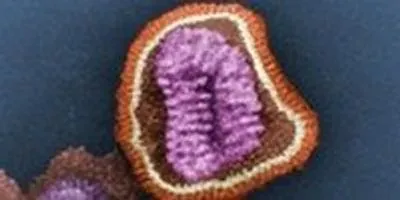
Influenza virion.Wikimedia, CDCIt’s a frustrating fact of life that coming down with influenza one year doesn’t guarantee anyone a flu-free season the next year. Even the flu vaccine doesn’t provide full-proof protection, as it covers only a select few strains of the virus—a selection that’s based on the World Health Organization’s best bet as to which strains around the world will be most prevalent in the coming flu season.
Influenza virion.Wikimedia, CDCIt’s a frustrating fact of life that coming down with influenza one year doesn’t guarantee anyone a flu-free season the next year. Even the flu vaccine doesn’t provide full-proof protection, as it covers only a select few strains of the virus—a selection that’s based on the World Health Organization’s best bet as to which strains around the world will be most prevalent in the coming flu season.
Unfortunately, those predictions are proved wrong about one time out of 20, explained Sarah Gilbert, who leads the Human Influenza Vaccine Programme at the University of Oxford’s Jenner Institute.
However, some researchers are getting closer to creating the ever-elusive universal flu vaccine, which could protect against a number of influenza viruses at once, including pandemic strains. If successful, universal flu vaccines would take the guesswork out of vaccine planning, and only require booster shots every few years.
One antibody to bind them all
Influenza is an RNA virus that uses its hemagglutinin (HA) protein like a key to allow it to enter and infect target host cells. In response to infection, or to a typical flu vaccine, the body produces antibodies that bind the head ...