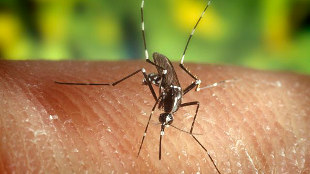
 The Asian tiger mosquito (Aedes albopicts) is a vector for many viral diseases, including dengue virus, which causes dengue fever, dengue hemorrhagic fever, and dengue shock syndrome.CDC, JAMES GATHANYT cells that specifically recognize dengue virus also express a surface marker that directs them to the skin, according to a study published today (March 11) in Science Translational Medicine. The discovery of skin-homing T cells could have important implications for dengue vaccine design.
The Asian tiger mosquito (Aedes albopicts) is a vector for many viral diseases, including dengue virus, which causes dengue fever, dengue hemorrhagic fever, and dengue shock syndrome.CDC, JAMES GATHANYT cells that specifically recognize dengue virus also express a surface marker that directs them to the skin, according to a study published today (March 11) in Science Translational Medicine. The discovery of skin-homing T cells could have important implications for dengue vaccine design.
“The concept that T cells are really going to be important for controlling natural dengue infection, and now in the context of dengue vaccination, is really big for the field,” said Sujan Shresta of the La Jolla Institute for Allergy and Immunology who was not involved in the research. “It’s really a paradigm shift.”
Dengue, a mosquito-borne infection that affects approximately 100 million people per year worldwide, comes in four different forms, or serotypes. Infection with one serotype provides lifelong immunity to that variant, but at most a year of protection from the other serotypes. After this period, secondary infection with another serotype results in severe disease. Researchers ascribe this puzzling response either to antibodies generated during the first infection or to T cells that ...






















